Tips on Bunion Care
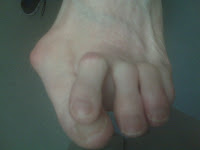
So you or someone you love is developing a bunion, what to do? Bunions are sometimes classified Stage I (you begin to see a bump), Stage II (the toe starts to drift towards the 2nd toe), Stage III (the 1st and 2nd toes come together), and Stage IV (the 1st toe moves under the 2nd toe with great instability to the entire foot as seen in the photo above). The goal of bunion care is to keep it in Stage II. During Stage II the bunion is not getting worse quickly since its alignment with the metatarsal is not too bad relatively. Stage IV is a surgical bunion and there are many great surgeries available. These surgical corrections, however, have a 6 month to 1 year recovery period depending on what is done.
Stage III can persist for 3 weeks or 30 years, and in general is a stable place for your overall foot stability. Once the 2nd toe begins to drift dorsally (towards the top of your shoe), Stage III can quickly become Stage IV. In Stage III, with the 1st and 2nd toes abutting, as you push off the ground at heel lift, the poor angle of the 1st toe pushes back on the metatarsal gradually increasing the bunion deformity over time.
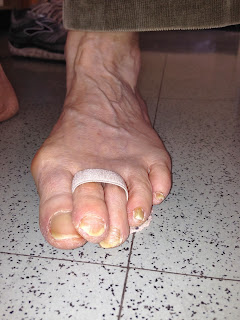
Sometimes a Budin Splint is used in Stage 4 to improve the overall stability. The success is based on the ability of the splint to keep the second toe at the same plane as the first. Here is a failure of the splint where the 2nd toe is too high off the ground.
So the goal in treatment is to get the bunion back into Stage II---its Happy Place, and keep it there. The bunion will not go away, but you may stabilize the joint, eliminating or at least postponing surgery for a long time. Bunion surgeries have not changed dramatically in the last 30 years like knee replacements, yet, the post operative care has greatly improved. I believe that avoiding/postponing surgery now, with the chance of never needing it, is worth the possibility of better results in the future. You will see this is my bias against immediate surgical procedures.
However, that being said, if you are disabled by anything like a bunion, try 6 months of aggressive conservative treatment first. If your condition has not improved after this time period, proceed with surgical advice. Your disability must match up with the risks and recovery period for the operation. Get 2 or 3 opinions, be a smart consumer, bring a friend or loved one to the appointments, make a logical decision, and go for it.
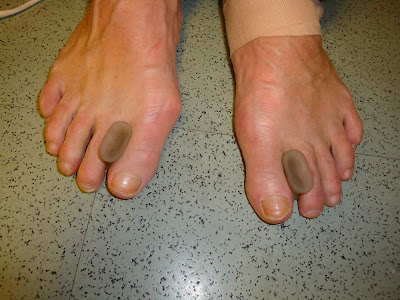
Stage II in bunion development is where, when you stand on the ground, and look at your toes, there is still a gap or separation between the 1st and 2nd toes. Medium gel toe spreaders from Silipos® http://www.silipos.com/ or separators between those two toes instantly put the bunion in stage II. You wear them in any enclosed shoe. You can now buy socks, like Injinji ® http://www.injinji.com/ , and bedroom slippers, like Vibram ® Five Fingers http://www.vibramfivefingers.com/ , that have individual compartments for each toe to wear around the house. Several years ago, YogaPro® came out with YogaToes http://www.yogapro.com/ . The product has 5 individual compartments and patients stretch their toes for 30 minutes 2 to 7 days a week when they are sitting down. I usually start patients at 5 minutes a day several times a week and they can slowly build up time. Some patients, especially with small toes, can not wear the product at all, or it must be modified. If you are in pain, do not wear the device (Good rule of thumb for most things). YogaToes are designed only to be used while sitting. Bed, Bath, & Beyond has an effective, but not as aggressive product, called Pampered Toes®. There is another YogaToes knockoff called Healthy Toes®. Another great product is Correct Toes where you can walk around with the toes in better alignment https://correcttoes.com/
Free standing Medium Gel Toe Separators, but I also like the Zenn Toe product that fits completely over the 2nd toe
If your bunion is red, start massaging it. The red inflamed tissue adds to the discomfort and fragileness in shoes. Use circular motion to try to get rid of unwanted inflammation with soft tissue swelling. Gradually push harder during the massage. Massage for 5 minutes several times a day for 2 weeks longer than you think you need. What do you massage with? Ice cube is used if the bunion is sore. If not sore, use massage oil, or any hydrating, lubricating, lotion or cream. It is the massage that moves out the bad stuff.
Padding with 1/4" adhesive felt just proximal to the bunion (called proximal padding) instantly takes pressure off of the bunion and allows you to wear many shoes that would normally irritate. The padding can be purchased in many locations including http://www.mooremedical.com/ item #09229. You normally cut out a 1 inch square and place not over the bunion, but just behind towards the arch, but as close to the bunion as possible. Best to place it on your foot directly. You can experiment with size and shapes so it does something without showing. You should never place under the foot or on the big toe itself—that will make the bunion worse. Sometimes, you may want to put on top of the 1st metatarsal and the side as just described. Each pad can be used multiple times, so 1 roll can last almost a lifetime or be shared with other bunion sufferers you know or see in the gym.
Another vital aspect to bunion care is strengthening of the intrinsic foot muscles. These are tiny, yet powerful muscles within your foot that weaken over time due to life stresses (the aging process, pain, bad foot mechanics, reliance on shoes and orthotic devices, etc.) Normally, I would send a patient to a physical therapist to learn these exercises properly.
If you can not wait, start doing the flatfooted balancing exercises now. All strengthening exercises should be done for a maximum of three days a week. Foot and ankle exercises fatigue the leg so much that they should be mainly done in the evenings when you are home for good. Stand on one foot in a doorway. Put your hands at your side so that you can grab the door frame if needed. Very slightly bend your knee that you are standing on. With your eyes open, try to balance on each foot for one minute until this is easy. Then, gradually build up to two minutes at a time. Then, begin to close your eyes during the two minutes off and on until you can keep your eyes shut the entire 2 minutes. This easy task can take 1 month to 1 year to complete. The longer it takes, the more important it is for you to accomplish this tremendous strengthening exercise. Very important: do not push through any pain whether it is in your foot, ankle, knee, hip or back. This is really where a physical therapist can help making sure you are safe at what you are doing. You can always have a doctor write a prescription and send you to therapy for 4 sessions to learn a HEP (Home Exercise Program).
In summary, bunion care should be started as soon as possible after making the diagnosis. Elements of treatment should include toe separators/spreaders, YogaToes or a knockoff version, proximal padding, possible socks and slippers with individual compartments, foot strengthening and massage. . Hope this was helpful. Of course, most of this advice is also used post-operatively to stabilize the strengthen the foot if it ever gets to that point.
Key Word: Bunion



Thanks.
ReplyDeleteThanks for taking the time to share this very helpful information.
ReplyDeleteThe main sign of a bunion is the big toe pointing towards the other toes on the same foot, which may force the foot bone attached to it (the first metatarsal) to stick outwards.
ReplyDeletewww.footsolutions.com