The following is an excerpt from Chapter 13 of "Secrets to Keep Moving" on Posterior Tibial Tendon Problems. It is an important tendon to protect. Yet, surgery in Stages 1, 2, and 3 can still be delayed or prevented if the doctors skill level can increase in conservative treatments. At least, you can have better informed conversations with your doctor after reading this.
7. Posterior Tibial
Tendinitis/Dysfunction/Tear
The posterior tibial tendon is the major tendon
to support the main arch of your foot. Damage to the tendon causes arch
collapse to a major degree. Any sign that this tendon is have problems must
therefore be over treated to avoid long term issues. It is one of the most common
surgeries on my patients because of the disability. I work long and hard on
each one of these patients both trying to avoid surgery (usually), or post
surgical rehabilitation.
https://youtube.com/watch?v=YPyC0ze2gO4&feature=shares
The top 10 treatments
for tibial tendinitis/dysfunction/tear are:
1. Understand the biomechanics of the
posterior tibial tendon to support the medial longitudinal arch and begin to
support the arch as part of all phases of the rehabilitation: Immobilization,
Re-Strengthening, and Return to Activity.
https://youtube.com/watch?v=7ilOVqF0aPc&feature=shares
2. Start with OTC and advance to custom
orthotic devices with maximal support (this is not an injury to have less than
optimal support).
3. Learn several different taping
techniques: posterior tibial and circumferential arch.
https://youtube.com/watch?v=AcSSyBfFocE&feature=shares
4. Ice the area 3 times daily for 15
minutes each.
5. If possible, get a baseline MRI (may be
an important comparison 6 months later), or baseline ultrasound imaging.
6. Most ankle braces hold the ankle
pronated which is bad for this injury, consider an Aircast Airlift PTTD brace
for times you are not using orthotic devices.
7. Create an initial pain free environment
with below knee removable boot/cam walker, and perhaps a Roll aBout knee scooter.
8. If the injury is substantial (Grade 3-4
typically), have a rigid AFO custom made at a brace shop right at the start of
the injury (it can take awhile to get fitted)
9. Begin strengthening the posterior
tibial tendon as quickly as possible with at least active range of motion
exercises. The Posterior Tibial tendon is strengthened by pointing the ankle
first and then moving the foot towards the other foot. See Chapters 2 (general
strengthening principles) and 6 (tendinitis principles).
https://youtube.com/watch?v=w3FXx4OFqec&feature=shares
10. Definitely have a surgeon as part of the
treatment, or the help of a regenerative specialist.
Email Correspondence
Patient: Hey Doc!!
I found your blog and I
am so grateful! I have already learned a great deal. I really need your advice
and help. Last fall I started to play tennis again. I played daily and began to
have foot pain.
Dr Blake's comment: When have taken time off from exercise, it is important to start
every other day so that you can access the toll on your body correctly, and
give yourself the 48 hours to regain your strength in your muscles.
Patient: The inside of my ankle
and the bottom of my foot were sore. In November I saw the ortho and he said I
had PTTD.
Impression Casts taken of a left sided PTTD showing the collapse inward of the heel and arch more than the right.
Dr. Blake's comment: Posterior Tibial Tendon Dysfunction diagnosis can be like shin
splints, you really do not know what is wrong by the name. The Posterior Tibial
Tendon is the most important tendon to support your arch. The Dysfunction part
implies that the tendon is not doing it's job, and patients have seen complete
collapses of the arch in severe cases requiring surgery. Since I do not know
the severity, but Melanie is implying that it seems difficult to treat,
therefore, to protect her, some immobilization must be recommended until more
info is obtained.
Patient: He put me in a walking
boot and that did not help.Dr. Blake's comment: This requires further information Melanie. The boot, like the photo
above, should have calmed the tendon down. Did it hurt just as much, 50%
as much, hard to tell? There are so many factors that come into play with your
injury. Normally, the below the knee boots are better than the mid calf or
ankle high ones. They distribute the force of stability over a larger area.
Also, with PTTD, normally wearing an arch support in the boot is crucial. If
you do not have a comfortable custom one, get the heat moldable Sole supports
soft athletic version. These are sold at sporting good chains like DIck's, REI, etc.
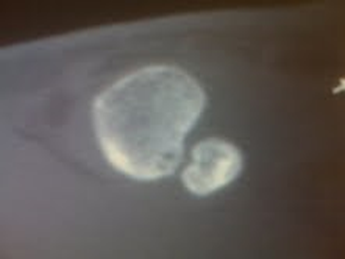
Patient: He also told me that I have an accessory navicular bone.
This CT Scan shows an Accessory Navicular, aka Extra Ankle Bone, aka Os Tibial Externum. Typically starts forming around 9 years old, and completely formed by 16. It can begin to give problems in young children in their early teens, or later in life.
This
extra bone occurs in a small percentage of people and normally weakens the
attachment of the posterior tibial tendon into the arch making it less
effective in supporting the arch and stabilizing the inside of the foot and
ankle.
Patient: It seemed to get worse.
( no arch or foot support in the boot). So off I went to the podiatrist.
He gave me an a shoe insert. It didn't help.
Dr Blake's comment: One of the very crucial points I need to make to all orthotic
wearers is why are you wearing them, and are they successfully fulfilling the
purpose they were prescribed? Why did you get the orthotics? Pain relief, or
better function? Orthotics if done well should make the posterior tibial tendon
work better, but maybe, just maybe, you are in the Immobilization Phase of
Rehabilitation, not the Re-strengthening Phase. So, a great orthotic device for
PTTD can make you hurt a lot more just because it is being used to stabilize
and re-strengthen at a time you should be immobilizing and using
anti-inflammatory methods. You are definitely in the removable boot with some
sort of orthotic and arch taping period.
Kinesiotape used for Circumferential Arch Immobilization
Patient: About a month ago, I
slipped in the kitchen and twisted the ankle on the same foot with the PTTD.
Since the initial fall I have rolled it two more times!
Dr Blake's comment: Once you hurt a major tendon, you body naturally protects itself.
You can roll your foot to the outside which makes you more prone to sprains, or
if a step will produce pain, you can just let the foot collapse/shut off and
you fall to the ground. These scenarios are quite common. And, if they are
happening to you, I can see why you emailed. It is very very frustrating.
Patient: I
look like someone beat me up! I keep spending money on shoes, inserts and
I need some advice. I started the tennis to lose weight, and I was.
Do I need a PTTD brace? I purchased some Orthaheel shoes but my
foot for some reason gets to a weird angle in them. I am doing the exercise you
recommend for strengthening my ankles. I know losing weight will help me, but I
need to know what to do so I can get back to tennis!
Thank you so much!!
Melanie (name changed
due to witness protection)
Dr. Blake's response:
Dear Melanie,
Thank you very much for writing. I hope some
of my initial comments were helpful. Please feel free to comment on this post
and I will try to respond in a timely fashion. To summarize:
#1
You are probably in Phase 1 of Rehabilitation:
Immobilization and Anti-Inflammatory where you try to create a Pain Free
Environment to let the tissue heal. We need to get you to that 0-2 pain
level range for 2 weeks straight.
#2
You can try combining the boot and orthotic, but may
have to get another boot or a different orthotic. You need to put out the time
and effort in creating this pain free environment.
#3
You should consider crutches, and even a Knee Scooter, for
a short time, if that is what it takes.
#4
For the Anti-Inflammatory part, definitely start ice
packing for 10 minutes three times daily. The ice pack can be placed in the
boot and you walk around (multi-task). Consider anti-inflammatory meds, flector
patches, and physical therapy for anti-inflammatory only (although you can send
me a video of you bouncing on the trampoline). LOL
#5
Normally, if the accessory navicular is the source of
pain, the pain will localize there as the symptoms die down.
#6
You should get (if possible) a baseline MRI or Ultrasound of the
ankle. It will show the rearfoot also, and may give clues to what is broken.
Hopefully, you strained but not tore the tendon.
#7 Since
tennis is out of the question right now, consider elliptical or stationary
bike, even some pool workouts will not irritate, as long as whatever you do
does not irritate the tendon.
#8
One important bit of information I need to further
advise regards pain. What produces it? How is it in the morning? See if you can
write up and email the pain questionnaire from Chapter 3. Also, go through the
various foot and ankle exercises described in my blog, at least the ones not
requiring equipment, and tell me which ones are painful and which ones are
symptom free. Go to YouTube and type drblakeshealingsole foot and ankle
strengthening playlist.
Further Email
Correspondences
Dear Yvonne, Thanks for
the email. I hope the video (go to YouTube and type drblakeshealingsole
posterior tibial strengthening exercises) helps you understand the 4 basic
forms of strengthening exercises used in the treatment of posterior tibial
tendon dysfunction. Gradually the patient is progressed from Active Range of
Motion to Isometric to Progressive Resistance to Functional. Heat (in the form
of warm water soaks, heat liniments, or heating pads) is used often to loosen
up the tendon before exercise for 10 minutes. If walking is not painful, 5
minutes of walking can get the blood pumping. Ice should be used after for 10
minutes, normally an ice pack over the sore area. NO Pain can be experienced
during the exercise. If you are still having trouble strengthening without
pain, try the numbing effects of ice. Ice the area for 5 minutes, then let the
tissue unthaw for 20 minutes, and then try the exercise. Should work unless the
tendon is significantly damaged. Then ice 10 minutes afterwards. I sure hope
this helps.
Rich
Further Email Answer
Patient: Dear Dr. Blake,
I have searched your
informative blog after not finding much on PTTD. I really enjoyed reading your
tailored approach to each patient in your blog comments, and I am hoping you
can give me some useful insights. I do like and trust my podiatrist, but I am
in a quandary and want to explore every avenue before entering into surgery.
Dr. Blake's comment: PTTD stands for Posterior Tibial Tendon Dysfunction. This is the
most important tendon for supporting the arch. Complete tearing of that tendon
always leads to complete arch collapse. So this is a very serious problem.
Patient: I am a 40 year woman in
excellent shape, trying to avoid surgery for PTTD. I found you in
reference to your use of inverted orthoses and I am wondering if the consistent
use of them might help me. I have consulted with two podiatrists and both have
agreed on the PTTD diagnosis, now I just need to figure out my plan.
Dr. Blake's comment: The Inverted Orthotic Technique is the most sophisticated foot
orthotic for arch support and is always used for PTTD. There are only a handful
of orthotic labs in the US that make them, but a relatively easy technique to
learn. Many labs now have versions of varus or inverted methods that can help greatly like the Mueller PTTD orthotic device. Before you try to find a lab with the Inverted, have the lab make the best possible orthotic device that they make for PTTD. Posterior tibial tendon acts across the foot and the ankle. A foot
orthotic will help the foot component, but at times, the ankle also must be
initially immobilized. In that case, you need a rigid AFO.
Patient: History and background:
I sprained both ankles
in my early 20's, the left ankle was a more severe sprain.
Dr. Blake's Comment: this probably left her with some weakness in her arch.
Patient: I have had pain in the
arch ankle area of my feet for the past six or seven years, always when wearing
improper footwear (heels). The pain always stopped when I went back to
supportive/comfortable shoes.
Dr. Blake's Comment: this is the classic presentation of PTTD where the symptoms begin
gradually in the arch and/or ankle areas.
Patient: I work-out in the gym
four times a week (weights, elliptical, stair climbing machine) and have always
hiked for exercise (usually once a week). My problem became severe when, on a
two-week trip in SE Asia in the Nov. '09, I wore flip-flops almost exclusively.
We did tons of walking, and at for the first time I noticed my feet burning and
tingling in the evenings. I did not connect this sensation to my other painful
flare-ups, because I had always assumed it was my high heels causing it. It did
not occur to me that I could hurt my feet wearing flip-flops.
Dr. Blake's comment: Again, the symptoms of PTTD gradually begin to change affecting
other activities, although one day of aggressive walking in flip-flops if you
have a predisposition can cause symptoms.
Patient: Over the next six months
I experienced increasing pain in both feet upon getting out of bed and standing
up first thing in the morning. My left ankle and arch started to look slightly
swollen, but I did not see a doctor.
Dr. Blake's comment: This is probably the first mistake, if you see swelling, the body is
actively trying to heal something, and may need some help and guidance.
Patient: I finally sought treatment
when, after a run last summer (August '10) , I was in so much pain in both feet
that I had trouble walking. I experienced shooting pains up the calves up both
legs at night and my left ankle and arch was red and painfully swollen.
Dr. Blake's comment: Here she is in the Immobilization/Anti-inflammatory Phase of
Rehabilitation. You must create a pain-free environment and allow the tendon
time to heal. You normally need a removable boot, followed by brace or AFO,
followed by orthotic device. You normally need to combine immobilization with
ice and contrast bathing to reduce swelling in the tendon. You normally begin
strengthening the tendon pain-free from the first visit. Emphasis on the
pain-free.
https://youtube.com/watch?v=rRt5hC24Afg&feature=shares
Patient: First podiatrist
diagnosed stage 1 PTTD and prescribed orthotics. Second podiatrist concurred
and added ice/anti-inflammatory therapy and in addition put me in a walking
boot until my inflammation subsided. After six weeks in boot I went to just
wearing the orthotics and sometimes Dansko shoes. My right foot felt 98%
better, and my left foot was improved to the point where I could often walk
with no pain (always wearing orthotics).
Dr. Blake's comment: Stage 1 the tendon is inflamed, but fully functional. Stage 2 the
tendon has some tearing, and begins to not support the arch well. Stage 3 the
tendon tears enough to not be functional, and the arch begins to collapse.
Stage 4 the tendon completely tears and the arch completely collapses
Patient: Which brings me to my
present situation; I am in pain a lot of the time once again, as sometimes want
to be barefoot (live at the beach, have a six-year old daughter), wear an
attractive (flat) sandal with support, but find that I cannot do so without
incurring a lot of pain in my left foot. As I write this I am back in my walking
boot as left inside ankle/heel area is throbbing with a dull pain. I wore shoes
without orthotic devices yesterday and I'm now paying the price!
Dr. Blake's comment: Golden Rule of Foot: Create a Pain-free Environment or else the problem
will not heal. This is especially true with PTTD. You need to create a pain-free
environment. You must stay in that boot until the pain goes away, and then add
another 2 weeks for good measure. I think one of the big treatments you have not mentioned is progressive posterior tibial strengthening. We need to make you strong!!
Patient: Upon hearing all of this
from me, my podiatrist has finally recommended surgery. He is of the opinion
that that is the only solution for my particular situation. I tend to agree,
but I feel overwhelmed when I hear the reality of the recovery. Is there any
chance he is wrong? Could I religiously wear the inverted orthoses and "heal"
my left foot the way my right foot was improved? Or should I just "suck it
up" and do the surgery so I can have a chance for a real recovery and a
lifestyle that will resemble "normal" again?
Dr. Blake's Comment: yes, yes, maybe
And Further Response to
same patient:
Thanks for the email. When patients present to my office
with this scenario, I just try to start over. Pretend the injury just happened.
Try to put a healing environment together for them to hopefully end with a
successful rehabilitation. Sometimes the decisions are hard to make, but we
make them and stand by them.
So, what must you do now? What will allow you to heal?
First of all, surgery is only needed at times for Stage 3 and 4. Does not sound
like you are there. Your focus must be immobilization, anti-inflammatory, and
re-strengthening. Nothing from this point on should hurt. The activities should
not hurt, the strengthening exercises should not hurt, and the physical therapy
should not hurt. Definitely read Chapter 2 on Good vs Bad Pain and live by it.
Since the posterior tibial is the strongest arch support
tendon, help it out as much as you can to do it's job. This is accomplished
with taping techniques, the Inverted Orthotic or similar protective orthotic device offered by labs, stable shoes, wedging of shoes,
power lacing, and bracing. Your podiatrist/therapist and you need to create a
stable environment, whether it is pre or post surgery. So if a surgeon does not
know how to create a stable environment for your tendon, if he/she does
surgery, they most likely will not know how to rehab it after.
Here are so many
strengthening exercises for the posterior tibial tendon that it is normally
easy to gradually build up the strength. Remember, if you try to strengthen a
muscle/tendon, and you produce a pain response, the tendon in the end gets
weaker. Since the posterior tibial tendon is next to the posterior tibial nerve, there may be some 0-2 pain that the therapist feels is acceptable, but it should have no increased pain afterwards.
https://www.drblakeshealingsole.com/2010/06/quick-tip-9-begin-strengthening.html
What helps control inflammation? Icing (if there is no
swelling or just after activity), contrast bathing if there is swelling, physical
therapy, acupuncture, many topical creams (some by Rx and some OTC), and oral
medications. I like to stay away from months and months of oral medications,
but short courses when the inflammation is flared is fine.
So Joann, my
recommendations for you right now:
- Stay in the Removable boot for
the left side until you can walk without pain for 2 weeks.
- Purchase an Even-up for the
right side to protect your back.
- Begin icing 3 times daily for
10 minutes both sides. The left should have evening contrast baths
starting at one minute hot and one minute cold alternating for 20 minutes due to the throbbing.
- Get an Inverted Orthotic Device
for both sides, or similar PTTD device per the podiatry lab, which is some type of orthotic that does not allow your foot to
pronate at all. You will need this to gradually wean off the cast.
- Begin some posterior tibial
tendon strengthening each evening followed by 10 minute ice bath.
- Get bilateral ankle MRI’s to
document June 2011 status of both your tendons.
- Find out the stage of your posterior tibial tendon
disease.
I sure hope this helps.
Rich