Welcome to the Podiatry Blog of Dr Richard Blake of San Francisco. I hope the pages can help you learn about caring for foot injuries, or help you with your own injury.
Total Pageviews
Translate
Followers
Wednesday, November 30, 2022
Arch Height In Custom Orthotic Devices
Tuesday, November 29, 2022
Sesamoid Injury: Cortisone Shot or Not?
Video On Designing Dancer's Padding for Big Toe Joint Problems
Monday, November 28, 2022
Video on Custom Orthotic Devices in the World of Biomechanics (from Dr Richard Blake)
Sunday, November 27, 2022
Video from Dr Richard Blake on Injury Rehabilitation General Rules
POSE Running: Video on the Basic Components
Saturday, November 26, 2022
Friday, November 25, 2022
Shock Absorption Problems: A Common Cause of Lower Extremity Problems
- Tibial Stress Fractures
- Knee Pain
- Calcaneal (heel) stress fractures
- Metatarsal stress fractures
- Heel Bursitis or Heel Bruise
- Femoral Stress Fractures
- Where there are many causes of poor shock absorption, patients who have excessive supination always have poor shock absorption. You need contact phase pronation to absorb the shock at heel strike.
Thursday, November 24, 2022
5th Metatarsal Fractures: A Special Breed (General Rules)
Fifth Metatarsal
Fractures: A Special Breed (by Richard Blake, DPM)
The top 10 initial treatments for 5th metatarsal
fractures are:
- X ray evaluation to decide on
surgery vs conservative care.
- If surgery, protocol to be set
by surgeon and not the purpose of this writing.
- If conservative care chosen,
some form of immobilization for 8-12 weeks is typically done based on
injury (Immobilization Phase). You want to get the pain level between 0-2 with 2 weeks, and maintain that during the entire rehabilitation.
- During the Immobilization
Phase, lower limb strengthening with some cardio should be orchestrated by
a physical therapist. Even one legged stationary bike is very beneficial.
- Bone health is analyzed with
dietary calcium and Vit D3, consideration of a bone density screen, and
typically healthy diet.
- Transition period from cast to
no cast, with or without surgery, can be very difficult. Custom orthotics
with full lateral arch support very helpful. At times, extra big shoes during the transition can be purchased so added padding/accommodation can be used.
- When not using a permanent
cast, 24/7 compression bandages, ice pack 15 minutes twice daily, contrast
bathing each evening, as much as possible elevation, 3 times daily 3 minute self massage for desensitization and swelling reduction, and hourly
pain free ankle circles are initiated.
- Weight bearing for bone mineralization,
even in casts or boots, is done as early as safe (Good Pain vs Bad Pain)
- All fifth metatarsal fractures,
except a few styloid process avulsion fractures, should have a Exogen Bone
Stimulator for 6 months (when insurance allows).
- Follow up xrays need only be
done when symptoms plateau or worsen. As long as the patient makes steady,
gradual, progress, it is better to base improvement on function, not x ray
or palpable tenderness.
A. Fifth Metatarsal
Fractures: Non Jones Type
These images are from
a patient of mine that is almost 3 months post injury and her x-rays show a
wide gap still. Here are all the thoughts that are meandering through my brain.
|
|
|
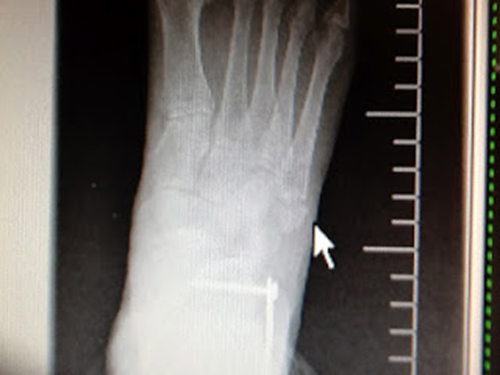
Here is the standard
Lateral view with quite a large gap noted |
|
|
|
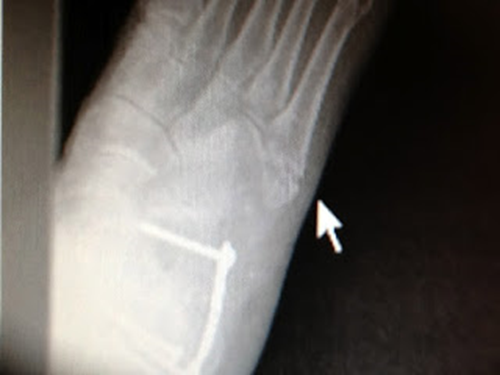
A Jones Fracture to
the Fifth Metatarsal is normally 1 inch closer to the toes. This AP view
still shows some displacement. |
|
|
|
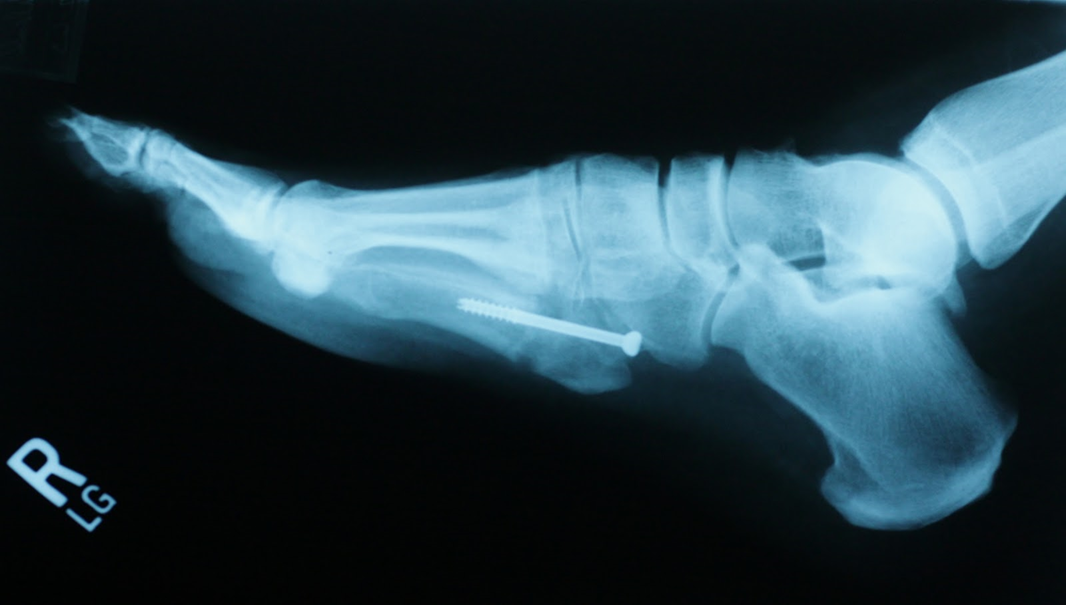
This Oblique view
makes the fracture clearer and you can see if the fracture line goes into the
joint of the 5th metatarsal/cuboid. |
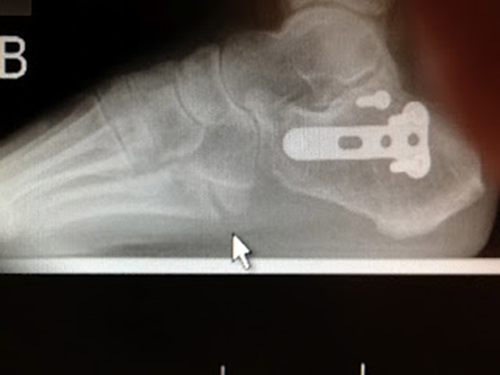
You can see in this post Jones fracture repair xray that the Jones fracture is further forward than a 5th metatarsal avulsion fracture.
This 5th metatarsal avulsion fractures following some inversion twist of the foot are typically under treated. Because they do not have the stigma of a true Jones fracture (historically more serious), they can be less aggressively treated. Sometimes this is okay, and sometimes not. Again, the goal is to create a pain free environment, which I believe has happened. X-rays for foot fractures, since the healing normally takes place internally first, cannot really reflect the strength of the bone. But, I do not like the gap and I do not like the fact that the joint is involved (possibly future arthritis).
So,
what are all the steps we need to make happen?
1) Establish a pain
free environment if not already occurring
2) Make sure Bone
Strength is good (questioning about Vit D3 and Calcium, bone density, healthy
diet)
3) Stabilize the fifth
metatarsal with orthotic devices, accommodative padding, and kinesiotaping
(there are special techniques in orthotic devices for the outside of your foot)
4) Set workout goals
that do not over stress this area
5) Avoid anti-inflammatories
since they can slow down bone healing
6) Ice Pack 15 minutes
twice daily, and contrast baths once daily to reduce inflammation
7) Due to the gap,
seek approval for Exogen Bone stimulator
8) Have patient talk
to a surgeon to find out what the process of fixing if the above does not work
(this keeps the patient well informed)
9) Advise on possible
future arthritis
10) Only get future X-rays if treatment has plateaued (there are many cases of pain free non healing) since current healing of the bone is not reflected well on x-rays.
Happy Thanksgiving from Drblakeshealingsole
Wednesday, November 23, 2022
Neuro One: Topical Medication for Peripheral Neuropathy
Hallux Rigidus: Position Paper on Treatment
- Make sure that the patient understands all surgical options
- Make sure that the patient is given a good opportunity to get the pain down to 0-2 VAS for 3-6 months before a surgical decision is made (a good attempt at conservative treatment)
- Make sure that the workup includes x rays and MRIs (even when the health plan does not pay for)
- Make sure that the patient understands that if they develop pain from compensating that they may need to be restricted to certain shoes and orthotic devices for the rest of their lives
- Make sure that patients are given the ability to talk to patients whose big toe joint fusions were over 5 years ago.
Tuesday, November 22, 2022
Subtalar Joint Neutral and Its Clinical Significance: Lecture Summary from the 10th Annual Schuster Memorial Seminar
- Positioning the foot and leg around subtalar joint neutral means that the stresses are even from medial to lateral
- Subtalar Joint Neutral is crucial in Repetitive Motion Activities
- Being too far from Neutral when functioning can cause pronatory or supinatory problems
- These problems can occur up the leg into the back, spine, and upper extremities
- Subtalar Joint Neutral has primarily a weight bearing significance
- Clinically it is observed from the alignment knee to foot or tibia to heel bisection (this is also called the TC or Achilles Angle)
- Most patients do not stand or walk in Subtalar Neutral due to variations in Tibial Varus or Valgus
- This variation gets more exaggerated when the varus or valgus starts in the knee (genu varum or genu valgum)
- Most podiatrists obtain stability in their patients by heel verticality
- Clinically it is important to know when this heel verticality is not close to subtalar neutral (on the pronated or supinated side) due to symptoms produced or not improved