Fifth Metatarsal
Fractures: A Special Breed (by Richard Blake, DPM)
The top 10 initial treatments for 5th metatarsal
fractures are:
- X ray evaluation to decide on
surgery vs conservative care.
- If surgery, protocol to be set
by surgeon and not the purpose of this writing.
- If conservative care chosen,
some form of immobilization for 8-12 weeks is typically done based on
injury (Immobilization Phase). You want to get the pain level between 0-2 with 2 weeks, and maintain that during the entire rehabilitation.
- During the Immobilization
Phase, lower limb strengthening with some cardio should be orchestrated by
a physical therapist. Even one legged stationary bike is very beneficial.
- Bone health is analyzed with
dietary calcium and Vit D3, consideration of a bone density screen, and
typically healthy diet.
- Transition period from cast to
no cast, with or without surgery, can be very difficult. Custom orthotics
with full lateral arch support very helpful. At times, extra big shoes during the transition can be purchased so added padding/accommodation can be used.
- When not using a permanent
cast, 24/7 compression bandages, ice pack 15 minutes twice daily, contrast
bathing each evening, as much as possible elevation, 3 times daily 3 minute self massage for desensitization and swelling reduction, and hourly
pain free ankle circles are initiated.
- Weight bearing for bone mineralization,
even in casts or boots, is done as early as safe (Good Pain vs Bad Pain)
- All fifth metatarsal fractures,
except a few styloid process avulsion fractures, should have a Exogen Bone
Stimulator for 6 months (when insurance allows).
- Follow up xrays need only be
done when symptoms plateau or worsen. As long as the patient makes steady,
gradual, progress, it is better to base improvement on function, not x ray
or palpable tenderness.
A. Fifth Metatarsal
Fractures: Non Jones Type
These images are from
a patient of mine that is almost 3 months post injury and her x-rays show a
wide gap still. Here are all the thoughts that are meandering through my brain.
|
|
|
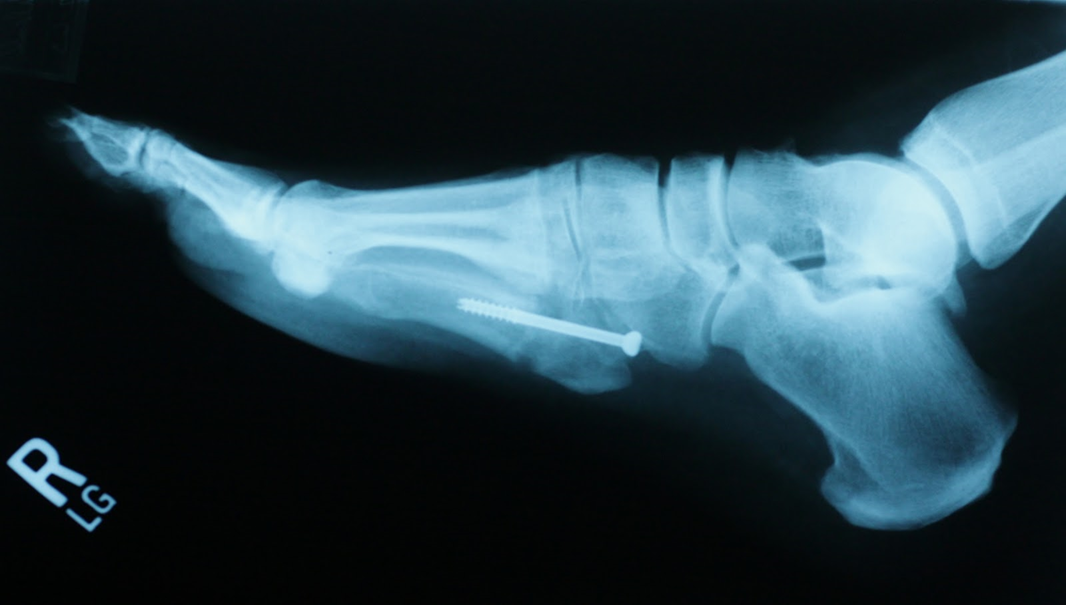
Here is the standard
Lateral view with quite a large gap noted |
|
|
|
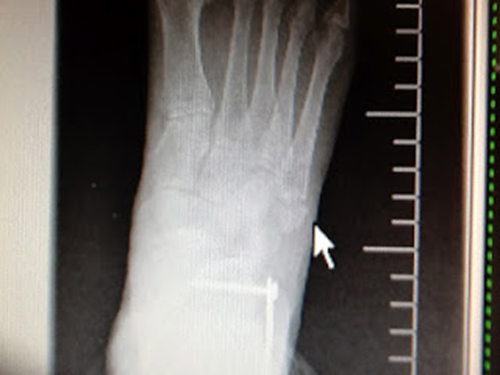
A Jones Fracture to
the Fifth Metatarsal is normally 1 inch closer to the toes. This AP view
still shows some displacement. |
|
|
|
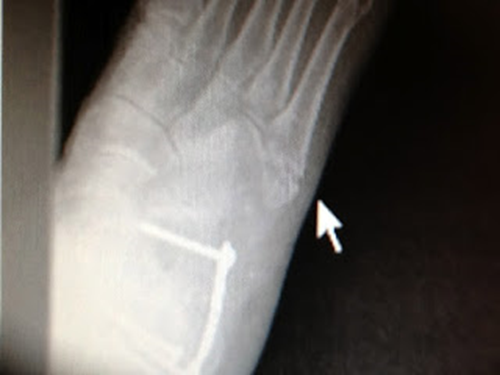
This Oblique view
makes the fracture clearer and you can see if the fracture line goes into the
joint of the 5th metatarsal/cuboid. |
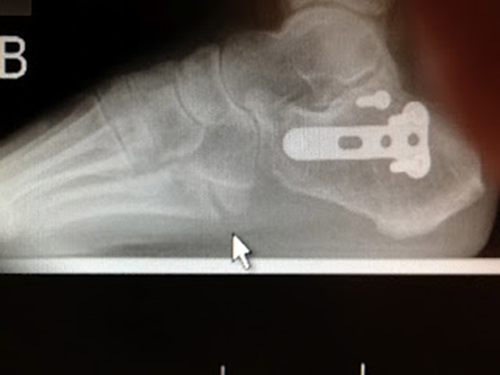
You can see in this post Jones fracture repair xray that the Jones fracture is further forward than a 5th metatarsal avulsion fracture.
This 5th metatarsal avulsion fractures following some inversion twist of the foot are typically under treated. Because they do not have the stigma of a true Jones fracture (historically more serious), they can be less aggressively treated. Sometimes this is okay, and sometimes not. Again, the goal is to create a pain free environment, which I believe has happened. X-rays for foot fractures, since the healing normally takes place internally first, cannot really reflect the strength of the bone. But, I do not like the gap and I do not like the fact that the joint is involved (possibly future arthritis).
So,
what are all the steps we need to make happen?
1) Establish a pain
free environment if not already occurring
2) Make sure Bone
Strength is good (questioning about Vit D3 and Calcium, bone density, healthy
diet)
3) Stabilize the fifth
metatarsal with orthotic devices, accommodative padding, and kinesiotaping
(there are special techniques in orthotic devices for the outside of your foot)
4) Set workout goals
that do not over stress this area
5) Avoid anti-inflammatories
since they can slow down bone healing
6) Ice Pack 15 minutes
twice daily, and contrast baths once daily to reduce inflammation
7) Due to the gap,
seek approval for Exogen Bone stimulator
8) Have patient talk
to a surgeon to find out what the process of fixing if the above does not work
(this keeps the patient well informed)
9) Advise on possible
future arthritis
10) Only get future X-rays if treatment has plateaued (there are many cases of pain free non healing) since current healing of the bone is not reflected well on x-rays.
No comments:
Post a Comment
Thank you very much for leaving a comment. Due to my time restraints, some comments may not be answered.I will answer questions that I feel will help the community as a whole.. I can only answer medical questions in a general form. No specific answers can be given. Please consult a podiatrist, therapist, orthopedist, or sports medicine physician in your area for specific questions.